by Elizabeth Carrollton
 Women who have experienced pregnancy and childbirth are significantly more likely to develop a condition called Pelvic Organ Prolapse. This condition is most commonly diagnosed when women are between the ages of 50 and 79, which is why Baby Boomer women should take careful note. While pelvic organ prolapse (POP) is not life-threatening, it can be incredibly uncomfortable in its most severe stages. There are several factors that make Baby Boomer women more susceptible to developing the condition.
Women who have experienced pregnancy and childbirth are significantly more likely to develop a condition called Pelvic Organ Prolapse. This condition is most commonly diagnosed when women are between the ages of 50 and 79, which is why Baby Boomer women should take careful note. While pelvic organ prolapse (POP) is not life-threatening, it can be incredibly uncomfortable in its most severe stages. There are several factors that make Baby Boomer women more susceptible to developing the condition.
Contributing Factors to Pelvic Organ Prolapse
Menopause
During menopause, women’s estrogen levels begin to decrease significantly. Collagen levels decrease as well, because estrogen helps to stimulate the production of collagen. Collagen is important for creating tissue strength and elasticity. Once collagen production slows down, skin and connective tissues become weaker and less elastic. In the case of pelvic connective tissues, this weakening can result in the development of POP.
Hysterectomies
Many women in the baby boomer generation were encouraged to get hysterectomies to treat a variety of reproductive ailments or as a treatment for ensuing menopause side effects. In fact, after C-sections, hysterectomies have been the second most common surgical procedure performed on women in the U.S. Now, OB-GYNs are discovering that the uterus is an essential component for keeping reproductive organs in place. As such, women who have received hysterectomies are more likely to develop a specific type of POP called vaginal vault prolapse.
Lifestyle
Smoking and obesity are also common factors in more severe cases of POP. Excess weight, and/or the strain of the chronic smoker’s cough, can put additional strain on pelvic ligaments and muscles. Over time, this strain compromised weakened tissues and can cause more severe prolapse.
Women can work to prevent the onset of POP by living a healthy lifestyle, including a healthy diet and regular exercise. Other preventative measures include:
- Pelvic exercises. Using pelvic exercises to strengthen the pelvic floor can prevent prolapse from progressing.
- Electrical stimulation. Doctors or physical therapists can use electrical stimulation to manually strengthen vaginal and pelvic floor muscles.
- Vaginal pessaries. Pessaries can be custom fitted and designed to treat specific symptoms. When inserted properly, they can prevent organ prolapse and reverse incontinence.
Surgical Intervention
In severe cases of POP, women may require the use of surgical treatments to reverse debilitating symptoms. Women should discuss surgical options with their doctor. One of the common surgeries is a vaginal mesh procedure. This treatment method has been linked to serious health problems. In fact, after multiple warnings from the U.S. Food and Drug 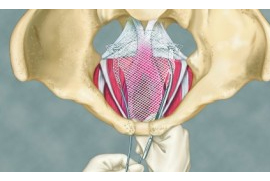 Administration (FDA), several manufacturers of transvaginal mesh have discontinued their products. Many have even recalled their vaginal mesh products and pulled them off the market.
Administration (FDA), several manufacturers of transvaginal mesh have discontinued their products. Many have even recalled their vaginal mesh products and pulled them off the market.
The highest numbers of complications are reported in mesh surgeries in which the mesh is inserted through the vagina. Surgeries that place mesh abdominally have fewer numbers of complications. Doctors can also perform surgery using natural grafting materials. These surgeries have fewer incidences of serious complications, as well.
The more women do to consciously focus on pelvic health, nourishing and strengthening pelvic muscles and tissues, the less likely they will be to develop POP or require more risky interventions.
Elizabeth Carrollton writes to inform the general public about defective medical devices and dangerous drugs for Drugwatch.com.
- http://www.uofmhealth.org/health-library/tv1000#tv1005
- http://www.cdc.gov/reproductivehealth/womensrh/hysterectomy.htm
- http://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm262435.htm
- http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm262752.htm
Winsome To Wisdom is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com
